Thoughts on canine pancreatic ultrasound and changes associated with pancreatic pathology
Ah pancreases, pancreases, pancreases…..I don’t think anyone finds it easy to get good views of all parts of the canine pancreas in all individuals. Deep-chested dogs, dogs with painful abdomens, gas in the duodenum and/or caecum are all confounding factors.
I find that using a high frequency linear probe is enormously helpful: the interpretation depend so much on tissue detail. My other discovery, over the years, is that good views can often be gotten in difficult circumstances with views through the dorsal parts of the intercostal spaces on the right. A transverse or oblique plane view is frequently useful.
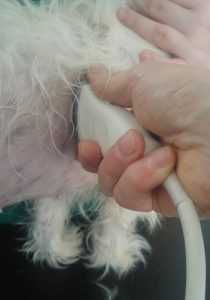
This should give a view something like:
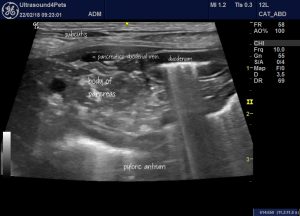
Oblique/transverse view of the body of pancreas and cranial duodenal flexure through an intercostal space on the right.
Which brings us to the thorny issue of what features suggest a diagnosis of pancreatitis?.
The always excellent Dominique Penninck in Atlas of Small Animal Ultrasonography (Blackwell 2008) gives us ‘In acute pancreatitis the pancreas appears enlarged and diffusely hypoechoic while the surrounding fat appears moderately hyperechoic’ and ‘in severe, haemorrhagic, necrotizing pancreatitis irregular hypoechoic areas represent necrosis and haemorrhage…. the pancreatic margins can be ill-defined and the pancreas and the pancreas appears amorphous’.
This is in line with published case reports:
‘All eight dogs with pancreatitis had an irregular, enlarged pancreas with a hypoechoic echotexture in six dogs and heterogeneous in two animals. The surrounding mesentery was hyperechoic in six dogs and anechoic free fluid was present in four dogs.’
Contrast-enhanced ultrasonography of the pancreas in healthy dogs and in dogs with acute pancreatitis.
Rademacher, Nathalie; Schur, David; Gaschen, Frederic; Kearney, Michael; Gaschen, Lorrie. Veterinary Radiology & Ultrasound. Jan-Feb, 2016, Vol. 57 Issue 1, p58
https://www.ncbi.nlm.nih.gov/pubmed/26332486
The problem is that all of these features are, to some extent, subjective. Pancreatic size is very variable and perception of echogenicity is machine setting-dependent and varies with changes in adjacent organs or presence of effusion.
Hypoechoic change in the inflamed pancreas is due to interstitial oedema. It’s not surprising then that acute pancreatitis can be hard to separate from alternative causes of oedema such as hypoalbuminaemia, portal hypertension or anaphylaxis. My suspiscion, increasingly, is that it can’t be done reliably.
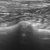
This is the left pancreatic lobe of a dog with hypoalbuminaemia due to protein-losing enteropathy (albumin 11 g/l) and a normal cPLI. It would be easy to make a diagnosis of pancreatitis here (and, in fact, I don’t have histopathology to rule it out). Abdominal fat around the pancreas is hyperechoic; the pancreas contrasts with it markedly and there are small pockets of peri-pancreatic free fluid.
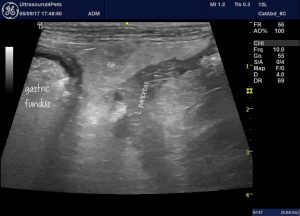
However, I have a strong suspicion that if you assessed the pancreatic parenchyma objectively you might find that it’s not dramatically abnormal. Dogs with severe chronic enteropathy often have hyperechoic abdominal fat. And the free fluid may well be due to hypoalbuminaemia.
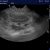
This is the right pancreas of the same dog including a loop of markedly abnormal jejunum:
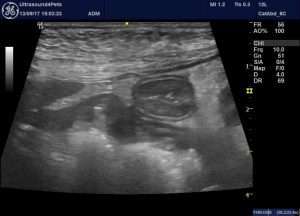
The hyperechoic change in the abdominal fat of this patient isn’t focused specifically on the pancreas; something I can’t easily show in a single image.
I have come across this PLE versus pancreatitis issue in quite a few patients. Having reviewed the literature I can’t find a convincing association between pancreatitis and enteropathy. My working hypothesis is that, most of the time, the enteropathy is genuine and a diagnosis of pancreatitis should be tentative.
Another potentially interesting scenario is anaphylaxis which can present as acute abdomen in dogs.
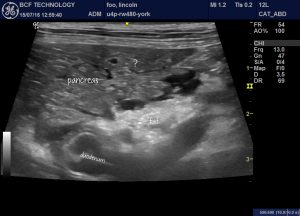
This is the body of pancreas of a dog who ran into a wasps nest, was stung multiple times, presented collapsed and recovered completely within 24 hours. In this case, the fat looks hyperechoic (I believe) due to small abdominal effusion. Again the pancreas is, arguably, not markedly hypoechoic.
It’s interesting to look at the human literature on acute pancreatitis.
‘Ultrasound is frequently the first investigation performed on admission; although it has little value in the diagnosis of pancreatitis or its complications’
Br J Radiol. 2010 Feb; 83(986): 104–112.
Imaging acute pancreatitis
B C Koo, MRCS, FRCR, A Chinogureyi, FRCR, and A S Shaw, MRCP, FRCR
In people, my understanding is that acute pancreatitis is generally diagnosed when two out of three criteria are satisfied:
- compatible history and physical examination
- elevated lipase or amylase
- compatible CT findings
We haven’t quite reached the same point with canine lipase/amylase assays unfortunately. Although reasonable theoretical argument suggests that cPLI should be specific:
http://vetmed.tamu.edu/gilab/research/pancreatitis-information
…there are still some unanswered questions about quite how often results are high in dogs with, for example, hyperadrenocorticism or enteritis.
The human perspective does cast a slightly different light on what we are doing in veterinary medicine when we ultrasound scan an acute abdomen. Maybe it’s not so much that we should feel able to make a positive diagnosis of pancreatitis in most cases: more that we are looking to rule out alternative (often surgical) causes of acute abdomen e.g. gastrointestinal foreign body, ruptured mucocoele, severe enteritis, septic peritonitis. I guess people probably don’t swallow kebab sticks as often as dogs! …..I might be wrong.
In fact, I wouldn’t characterise ultrasound as being ‘of little value’ in confirming a diagnosis of acute pancreatitis in dogs. I would contend that this:
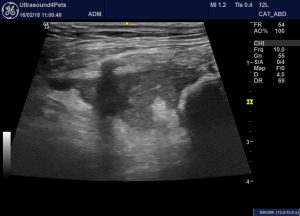
…is pretty much pathognomonic. There is local swelling of the tip of the right lobe in this patient an adjacent fluid accumulation and marked, localised hyperechoic change in the fat. Other systemic diseases don’t cause such focused changes.
Another feature which makes me really suspicious of pancreatitis -and which I believe probably indicates chronicity (sonographic features of chronic canine pancreatitis have not been published to the best of my knowledge) is patchy hyperechoic ‘marbling’ within a diffusely hypoechoic pancreas. In my experience this is not a feature of other causes of pancreatic oedema.
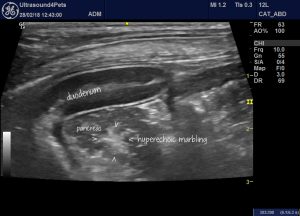
Oblique view from the right 11th intercostal space showing the cranial duodenal flexure with the body of pancreas. The pancreatic parenchyma is, subjectively, hypoechoic but marbled with hyperechoic patches. This dog had suffered multiple episodes of cPLI +ve pancreatitis over several years and was scanned during a flare up.
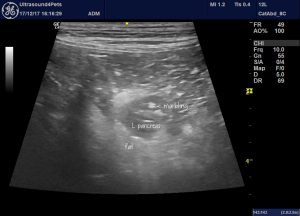
Another example of hyperechoic marbling. A longitudinal plane view of the left lobe of a cPLI positive dog with acute vomiting and no obvious alternative causes.
Since this is turning into a bit of a ramble through all aspects of pancreatitis…this is the oedematous stomach wall of the same dog. I’ve seen this before in occasional cases.
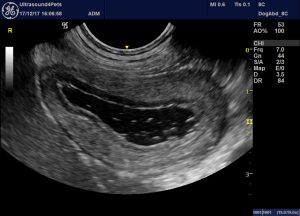
longitudinal plane view (i.e. short axis view of the stomach) of the gastric body of the same dog. The oedema is dramatic.
And finally…
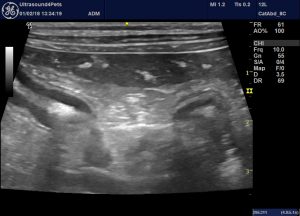
Right flank long axis view of the right lobe of pancreas (and loops of jejunum). Athough the adjacent fat isn’t dramatically hyperechoic the pancreatic parenchyma does look hypoechoic. This contrasts markedly with hyperechoic foci within the right lobe. This is a cPLI negative dog with diabetes mellitus.
According to this interesting recent article….
Extreme Beta-Cell Deficiency in Pancreata of Dogs with Canine Diabetes
By: Shields, Emily J.; Lam, Carol J.; Cox, Aaron R.; Rankin, Matthew M.; Van Winkle, Thomas J.; Hess, Rebecka S.; Kushner, Jake A.. In: PLoS ONE. June 9, 2015, Vol. 10 Issue 6
http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0129809
…pancreatitis is rare in diabetic dogs. Histopath findings suggest targeted immune-mediated destruction of islet cells.