The role of sonography in feline urethral obstruction and the magic of cisatracurium
Urethral obstruction is another of those scenarios where ultrasound is under-used. Like azotaemic cats, I feel that they pretty much all benefit from being scanned.
This is a recent patient, a male cat obviously, 24 hours after a difficult unblocking and who still has an indwelling urethral catheter.
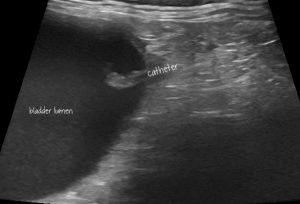
Longitudinal plane view of the bladder neck with catheter in situ
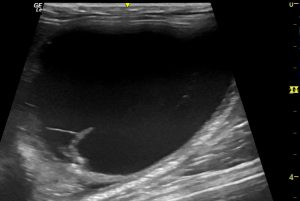
Longitudinal plane view of the bladder: there is a network of strands traversing the lumen, no obvious calculi (perhaps some mineralisation within the strands) and no obvious mass lesions
Several things to take from this:
The bladder is full: it’s not emptying through the indwelling catheter.
The tip of the catheter is blocked by a plug of non-mineral material (mucus, clot)
The catheter is in the desired place: it’s long enough to reach the bladder, isn’t (currently) perforating the urethral wall and there’s no effusion around the bladder neck to suggest uroabdomen (a common finding in this situation due to either bladder rupture, iatrogenic perforation of urethra or bladder with the catheter or post-cystocentesis).
It doesn’t look as though this cat has a urolith problem. I would be thinking that idiopathic cystitis is the prime differential.
Those ‘strands’ across the bladder lumen are usually organised fibrin adhesions arising as the sequel to previous episodes of urethral obstruction with bladder wall compromise. So called ‘pseudomembranous cystitis’.
https://www.mdpi.com/2306-7381/8/7/125/pdf
More detail of the proximal urethra:
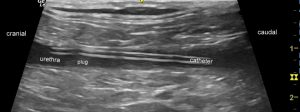
Longitudinal plane view of the proximal urethra in the same cat
OK, we know that the catheter isn’t patent. In this view we can see that the proximal urethra around the catheter is also dilated. That implies that the part of the urethral lumen not occupied by the catheter may also still be obstructed. Furthermore, there’s actually a non-mineral plug visible sitting in the lumen. This is a very common scenario: at the time of catheterisation the catheter has been pushed past the obstructing plug…but it hasn’t been retropulsed into the bladder and remains in situ. There’s a very high probability that this cat will re-obstruct in short order if the catheter is removed -and this will be the case whether you leave it in for 24 hours or for 3 days.
Another case to illustrate the point, courtesy of the lovely team at Yorkshire Vets: cat with urethral obstruction, catheterised without meeting any resistance and bladder drained uneventfully. Catheter subsequently removed. This is the post-procedure radiograph:
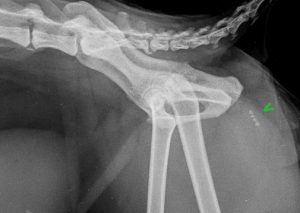
Oxalate calculi in the urethra of a cat. A urinary catheter passed straight over these and they remained in situ after removal of the catheter. This is the post-procedure radiograph!
Very commonly this leads to successive episodes of catheterisation, de-catheterisation and re-obstruction: leading to perineal urethrostomy.
The solution to this is to drain the bladder via the catheter (we flushed the plug out of the tip first), remove the catheter, infuse a muscle relaxant into the urethra via a catheter positioned with the tip just inside the penile urethral orifice. Wait five minutes and then, with the catheter in the same position, flush through the urethra vigorously with 20ml sterile saline into the bladder. Pass the catheter gently to the bladder, drain and then repeat the flush/drain cycle 5 or 6 times. In the vast majority of cases this will retropulse any remaining urethral plug and the residual relaxation of the urethra prevents spasm. This means that the catheter can be removed, the buster collar can be taken off, the cat can pass urine and everyone can relax. If the cat will tolerate it without anaesthesia, I often flush the urethra with another dose of muscle relaxant 12 hours later.
Obviously this doesn’t com with guarantees. However, in the last 8 years or so since the publication of the seminal…
J Small Anim Pract 2012 Jul;53(7):411-5
Effect of intraurethral administration of atracurium besylate in male cats with urethral plugs
F Galluzzi 1, F De Rensis, A Menozzi, G Spattini
https://pubmed.ncbi.nlm.nih.gov/22747734/
…I can’t remember having to submit more than one blocked cat to urethrostomy. Obviously, if you’re retropulsed calculi into the bladder then a cystotomy may be required.
Despite the fact that atracurium appears, in our experience, to be safe and largely effective, our observation is that it’s not widely used in veterinary practice in the UK. An observation supported in a recent review:
Can Vet J. 2020 Jun; 61(6): 595–604.
In-hospital medical management of feline urethral obstruction: A review of recent clinical research
Kevin L. Cosford and Siu To Koo
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7236633/
Who say….
‘Further investigation is needed to understand the efficacy and safety of this novel approach.’
Galluzi et al. used atracurium which was available under the trade name ‘Tracrium’. In the last couple of years this has become increasing hard to source. Instead we have been using Cisatracurium: available as a generic. We buy this through our local pharmacy. I’m not aware that veterinary wholesalers routinely stock it.
https://bnf.nice.org.uk/medicinal-forms/cisatracurium.html
As far as I can tell, the potency of cisatracurium is three times that of atracurium on a milligram for millgram basis.
Saudi J Anaesth. 2010 Sep-Dec; 4(3): 152–157.
Cisatracurium in different doses versus atracurium during general anesthesia for abdominal surgery
A. M. El-Kasaby, H. M. Atef, A. M. Helmy, and M. Abo El-Nasr
‘The neuromuscular blocking potency of cisatracurium (NIMBEX) is approximately three-fold that of atracurium besylate, the time to maximum block is up to 2 min longer for equipotent doses of NIMBEX compared to atracurium besylate. The clinically effective duration of action and rate of spontaneous recovery from equipotent doses of NIMBEX and atracurium besylate are similar.’
And that’s how we’ve been using it. To save you the calculation we administer 4ml of 0.15mg/ml cisatracurium (diluted in saline) at each per-urethral dose.
You don’t really need me to tell you that it’s not licensed in veterinary species. The obvious caveats apply: we have only trialled this in a few cats. However, we haven’t observed any adverse effects and, subjectively, it seems to be as effective as atracurium.
It’s not expensive. Personally, I think it’s an indispensable part of the pharmacy of all practices. We haven’t really discussed in this article how much easier and safer (less risk of iatrogenic trauma or rupture of urethra) it is to unblock a male cat using muscle relaxation with atracurium/cisatracurium. Read the Galluzi paper: You never need to struggle for half an hour again.
‘mean time required for the removal of the urethral obstruction was significantly shorter in the treatment group than in the control group (21·1 ±16·2 seconds versus 235·2 ±132·4 seconds; P<0·001)‘