An acute enterocolitis in cats with striking sonographic features: is this a novel disease entity?
In recent years I’ve seen a series of cats with a striking syndrome of acute, severe diarrhoea of unknown cause. The more I see of these; the more I’m suspicious it’s a disease entity which isn’t fully described in the published literature. The three recent cases described below are typical representatives of the phenomenon.
All were previously healthy, vaccinated, adult cats with access to the outdoors who suffered acute, profuse, watery diarrhoea and fever, occasionally with some vomiting, all resulting in profound malaise/weakness/lethargy. Two cats were icteric with normal liver enzymes and haematocrit. None were neutropenic: two showed moderate neutrophilia. Two cats were moderately thrombocytopaenic.

Severe watery diarrhoea in case 2

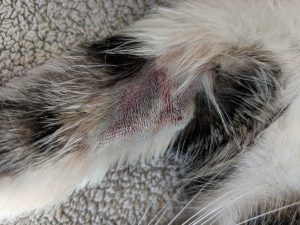
Disproportionate bruising at cephalic venepuncture site: case 1. Like many affected individuals this patient exhibited multiple features of sepsis. Platelet count was markedly subnormal (40,000/ul)
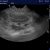
On sonography the dominant finding in all three was diffuse large intestinal wall thickening with a small amount of liquid content and gas bubbles:
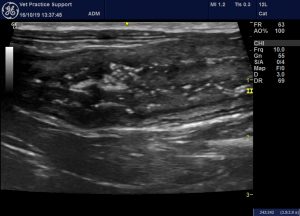
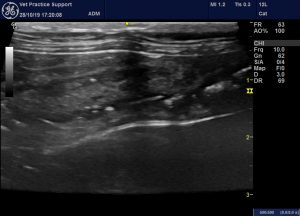
Longitudinal plane views of the left, descending colon from cases 1 and 2 showing dramatic, diffuse wall thickening with scanty liquid diarrhoea and gas bubbles. All of these cats recovered fully within a couple of weeks (it’s not lymphoma!)
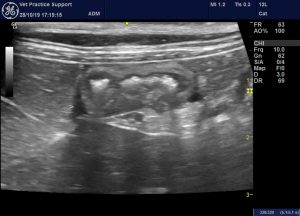
transverse view of the left (descending) colon in case 2. Adjacent fat is hyperechoic and there are very small pockets of free fluid

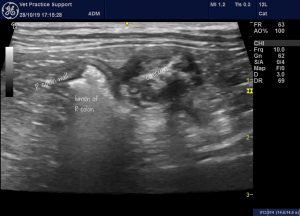
case 2 -the caecum is also affected
 Small intestinal changes were also a feature. In cases 1 and 2 they were relatively mild: diffusely increased mucosal echogenicity and increased volume of liquid content.
Small intestinal changes were also a feature. In cases 1 and 2 they were relatively mild: diffusely increased mucosal echogenicity and increased volume of liquid content.
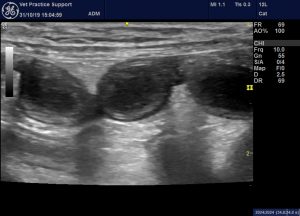
jejunum case 3
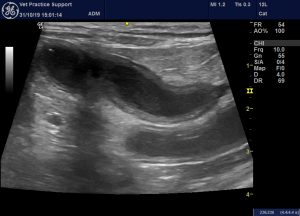
jejunum case 3 long axis

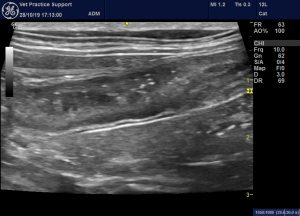
jejunum case 2

This functional ileus is also reflected in gastric dilation:
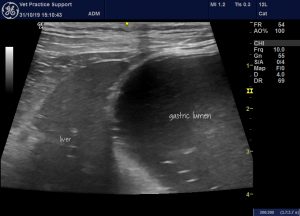
A dilated, amotile stomach in case 3

Gut-associated lymph nodes are moderately enlarged, rounded and contrast with mildly hyperechoic peri-nodal fat:
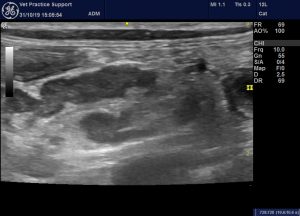
Jejunal nodes case 3
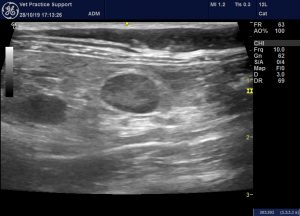
a prominent caudal mesenteric node from cat 2

Lungs and remaining abdominal organs were largely unremarkable sonographically.
Treatment and outcomes:
All three cats received intravenous fluids, maropitant, co-amoxiclav. Sometimes with opiates and metoclopramide. One was fed by oesophagostomy tube. All three made a full recovery within 10 days after hospitalisation for 7, 3 and 8 days respectively. Faecal tests for Campylobacter, Salmonella and Giardia proved negative in all cases.
Discussion:
Over the years I have seen occasional patients with similar presentations. I’m increasingly suspicious that this is a disease entity which isn’t really described in the literature. These cats appear to suffer an acute enterocolitis with systemic signs and clinico-pathological findings consistent with sepsis as described by Brady et al. (2000). Specifically, icterus in cats in the absence of anaemia or elevated liver enzymes is most typical of either sepsis or FIP.
Given that all three of these recent cases were full vaccinated, adult and had normal/raised neutrophil counts, panleucopaenia seems highly unlikely. The possibility of virulent systemic calicivirus bears consideration. However, they lack the spectrum of signs usually associated with VS-FCV (high mortality rate, oedema, skin and oral ulcers, hepatitis, pancreatitis, pneumonitis).
There is a single report of acute enterocolitis in cats in the USA which was associated with the presence of Anaerobiospirillum bacteria. However, a high proportion of those cats had concurrent illnesses and 5/6 cases were fatal. A causal role for Anaerobiospirillum has not been proven with transmission studies and remains putative.
Despite presenting with collapse to the point of near-recumbency, all three of the cases documented above recovered fully. In fact, to the best of my knowledge, none of the cats which I have seen with this syndrome have died from it. In many aspects of sonography, presentation and the epidemiological pattern of sporadic appearance in single cats, this is more like acute haemorrhagic diarrhoea syndrome (AHDS) or haemorrhagic gastroenteritis (HGE) in dogs -except less haemorrhagic.
Recent work has provided further support for the long-proposed role of Clostridia in canine AHDS (Gohari et al. 2015). Specifically, strains producing a novel spore-forming toxin (coded by the netF gene) appear to be associated with disease. I haven’t yet had the chance to submit samples from affected cats for netF testing but it’s an interesting area to look at. The GI Lab at Texas A&M offers the test.
References:
Brady et al. Severe sepsis in cats: 29 cases (1986-1998). J Am Vet Med Assoc. 2000 Aug 15;217(4):531-5
Gohari et al. A Novel Pore-Forming Toxin in Type A Clostridium perfringens Is Associated with Both Fatal Canine Hemorrhagic Gastroenteritis and Fatal Foal Necrotizing Enterocolitis. PLoS One. 2015 Apr 8;10(4)
Hi Roger
Thanks for your interesting cases
The pictures on this case seem to be absent 🙂
Would be interesting to do faecal PCRs on these cats- I have seen a couple of severe/per acute enterocolitis cases which required hospitalization too – with similar intestinal thickening. I don’t have follow up but clinical symptoms ameliorated and and the cats did not return for further diagnostics following discharge….
Best wishes
Rajat
Thanks Rajat, Hopefully the images are back again! Yes, I’m hoping to get some PCRs for netF done in the near future. Texas A&M ask for samples preserved in ethanol when sending internationally. I didn’t always ave any ethanol with me in the past when I saw these cats.